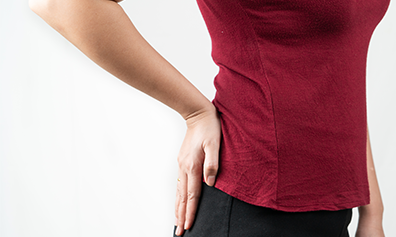
In today’s world, increased sedentary workstyle, gaming, and technology have reduced activity levels, causing back pain to become a common occurrence in young adults and the older population. Given the various potential underlying factors that lead to back pain, it makes sense to delve deeper into understanding them to help ourselves heal better from this modern age curse.
Pain is an unpleasant stimulus, and the response to this stimulus varies from person to person. For example, a mild strain might cause excruciating back pain, while there might be no pain in another individual with disc extrusion. There might also be potential underlying factors that might cause intermittent flare-ups of pain. Since the pain is subjective and varies in type and intensity, it is always advisable to actively participate in the treatment protocol to ensure the most successful outcome.
Understanding the causes of back pain
The back is complex, and the pain issues might be related to orthopedic or neurologic causes. For example, the spine undergoes much stress through activities like twisting, turning, bending, sudden jerky movements, etc. If the mechanics used during these activities are not ideal, it might result in back pain.
The orthopedic factors associated with back pain can be:
- • Injury to joints, ligaments, muscles, and bones of the back.
- • Strain to the larger muscles of the back.
The manifestations, however, are interconnected, and predisposition to one may lead to another.
Orthopedic Factors:
- • Injury to bones, joints, ligaments, or muscles of the back
- • The strain of the large muscles at the back
Neurologic factors:
- • Spinal cord injury
- • Disc protrusion/herniation
- • Nerve impingement/irritation
Degenerative changes in the orthopedic structures might eventually lead to neurologic signs and symptoms accompanying back pain depending upon the structures involved.
Identifying the causes of back pain:
The right diagnosis of the cause of back pain is paramount to fixing the issue so that pain resolution can occur. However, the complexity of the back with the several structures involved and them sharing common nerve supply adds to the complexity of making the right diagnosis.
The following steps are a good plan to move in the right direction regarding the diagnosis:
- • The individual needs to be interviewed to attain their medical history and the present history about the present issue of back pain with details about the onset of pain, the type of pain, and the intensity of pain experienced.
- • An objective examination needs to be conducted with detailed physical and special tests that would help rule out and rule in structures that might be the issue.
- • Further diagnostic tests in the form of X-rays and MRI might be advised depending upon the structures suspected to be involved.
- • When a definite etiology is not found, symptomatic treatment and conservative care are provided to help manage the back pain.
The most common types of back pain experienced are:
- • Mechanical pain: Usually precipitated by muscle strains and can be sharp or dull, intermittent or constant.
- • Referred pain: Dull and achy pain experienced at a location away from the actual region of the issue. For, e.g., Degenerative disc disease may produce referred pain along the course of the nerve impinged or irritated without actually causing back pain.
- • Radicular pain: Deep pain along the course of nerve with possible weakness and loss of sensation. It is caused by injury to a spinal nerve root, irritation, or compression by the surrounding structures. Some common underlying conditions causing radicular pain include sciatica, spondylolisthesis, disc degeneration, and spinal stenosis.
Managing back pain
The first line of treatment in self-management of back pain usually includes:
- • Pain medications as required
- • Anti-inflammatory and analgesic ointments
- • Heat therapy
- • Correction of faulty posture and maintaining good posture
- • Using relaxation techniques to relax the muscles that might be tight and causing the pain
- • Strengthening the weak structures and muscles
- • Stretching the tight structures and muscles
- • Modifying the activities to ensure they are being completed without eliciting pain
- • If the pain lingers even after the above self-management, consult a specialist to rule out issues that might have the potential to cause long term disability due to their severity
In conclusion, managing back pain is easier, and the healing process is faster if taken earlier than later. The later you push this pain resolution, more structures might get involved and prolong the healing process.